Rooted in Results Let’s Get Growing
Hair loss is a symptom. We begin every journey by finding the cause, so your treatment plan isn’t just hopeful—it’s strategic, personalized, and proven to work.
Contact Our Team
Scarring Alopecia is a type of hair loss that occurs due to inflammation around the hair follicles. The inflammation causes scarring in the affected area, leading to the destruction of the hair follicles and ultimately causing permanent hair loss. Scarring Alopecia can affect anyone regardless of gender or age. However, this type of hair loss is much more common in women than men, with some studies reporting as high as a 4:1 ratio of women to men.
While still a more rare type of hair loss, over the years we have seen an increase in the number of patients experiencing scarring alopecia. Patients diagnosed with scarring alopecia now make up over 10% of our practice. While part of the reason for this is that the medical community is becoming better at identifying, we also do believe that the incidence of scarring alopecia is increasing. There is some evidence to suggest an autoimmune cause, and there may be a genetic component as well, but more research definitely needs to be done.
There are several types of scarring alopecia, each with their own distinct characteristics and treatments. The most common types of Scarring Alopecia are Central Centrifugal Cicatricial Alopecia (CCCA), Lichen PlanoPilaris (LPP), and Frontal Fibrosing Alopecia (FFA).
The cause of scarring alopecia is still not fully understood. There is some belief that chemicals in cosmetics could be playing a role, but more research needs to be done. It is believed that there is a genetic component that makes certain people predisposed to these conditions.
The symptoms and presentation will differ depending on the type of scarring alopecia. However, patients may experience rapid hair loss in certain areas of the scalp. Some patients will also experiencing burning of the scalp, which is due to the inflammation on the scalp. The presentation of the hair loss will differ depending on the type of scarring alopecia:
After completing a medical history and initial physical exam, the next step in evaluating for scarring alopecia is conducting trichoscopy, which is a highly magnified camera that looks at the hair follicles and scalp at 30-60x magnification. Trichoscopy allows the hair loss specialist to see specific attributes that cannot be seen with the naked eye.
With many patients, a diagnosis can be made after completing the trichoscopy, however, in some cases to ensure a definitive diagnosis a scalp biopsy may be recommended. A scalp biopsy is a simple procedure where a 4mm punch of scalp is removed and sent to a dermatopathologist that can provide further testing of the hair follicles. A scalp biopsy will provide a definitive diagnosis if the patient has scarring alopecia and which type of scarring alopecia.
It is important to understand that scarring alopecia can cause permanent hair loss if not treated early and aggressively. The inflammation around the follicles can actually destroy the follicles and scar around them. The first goal of treatment is to stop the inflammation. This can be done through a combination of topical and oral steroids, prescription medication, and low-level laser therapy (LLLT). Once the inflammation has subsided, the goal of treatment could be shifted to try to regrow some of the hair.
Scarring alopecia is a very aggressive disease. The outlook and prognosis is going to depend on how much loss has already occurred and how long the patient has been experiencing the condition. With our updated treatment protocols, we are getting much better at stopping the progression of hair loss and in many cases seeing some regrowth. Unfortunately, none of the treatments for scarring are curative. This means the patient will need to continue to be monitored and treatments will need to be maintained.
The initial treatment regiment for scarring alopecia is based on stopping the inflammation. This is typically accomplished using a combination of topical and oral medications, as well as low-level laser therapy (LLLT). Once the inflammation is under control and the hair loss has stabilized, treatment for regrowth can be considered, which could include low-level laser therapy, if not already on it, platelet rich plasma (PRP) therapy, and possibly hair transplants.
Topical or injectable steroids are often one of the first treatments recommended for scarring alopecia. Clobetasol is a topical steroid that can be used for larger areas and Kenalog injections can be used for smaller areas.
Historically, two of the more common oral medications used for scarring alopecia are hydroxychloroquine and doxycycline. These are utilized due to their anti-inflammatory affects, but they also have significant potential side effects that need to be carefully monitored.
More recently, we have begun using low dose naltrexone (LDN) as an alternative anti-inflammatory oral medication. This medication is very well tolerated and we have seen very good results on it. However, the research on LDN is mixed and more research is needed.
Low-level laser therapy is a great additional treatment for scarring alopecia. Studies have shown that LLLT decreases inflammation, which is the first goal of treatment. LLLT is also a preferred treatment option for restoring the hair once the inflammation has decreased. This allows the healing process to begin while treating the inflammation.
Platelet Rich Plasma (PRP) Therapy is a simple in office treatment where concentrated amounts of the patients own platelets and growth factors are injected into the scalp. It has been shown to repair and rejuvenate hair follicles. Typically, PRP is not a first line of defense with scarring alopecia. It would not be used until the inflammation has decreased and the hair loss has stabilized. However, research is being done to see how scarring patients respond to PRP therapy. Recently, an article was published about a patient that had successful treatment with a combination of PRP and low dose naltrexone.
When there is significant loss from scarring alopecia, hair transplants can be an option to bring hair back to those areas, but it is not possible to transplant into an area that is actively inflamed. A hair transplant would not be recommended until the area has been inactive for at least one year and ideally two.
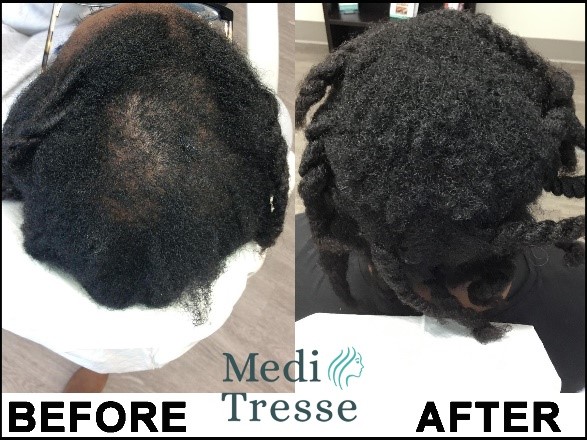
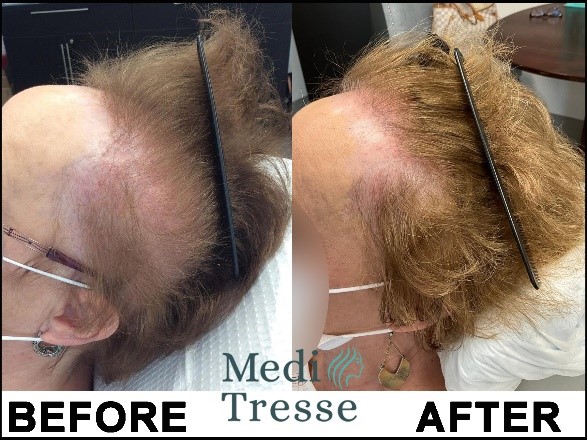
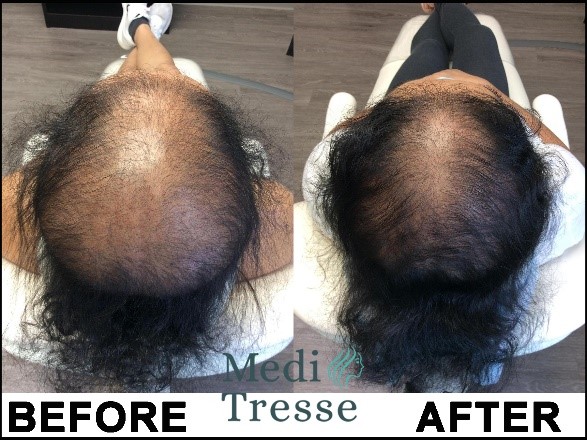
While results will vary depending on each patients situation and duration of their hair loss, we have had a lot of success treating this type of hair loss. As scarring alopecia patients now make up over 10% of our patient population, we have a lot of experience dealing with these types of hair loss and ensuring we can provide the best possible treatment regiment.